Sleeve Gastrectomy
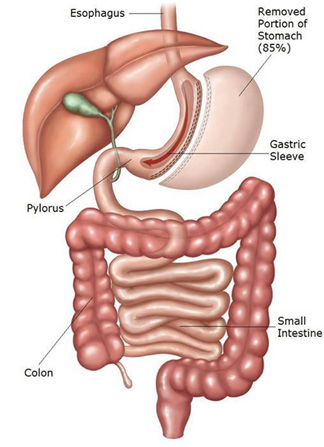 A procedure in which a stapling device is used to create a thin vertical sleeve of stomach about the size of a banana and the rest of the stomach is removed, thereby limiting the amount of food that can be eaten. It basically leaves a small stomach tube instead of a big stomach sack. The residual stomach capacity is about 150mls so a generous entry should be possible. Grehlin, which is an enzyme produced in the fundus of stomach, is responsible for hunger and craving for food. In this operation, Grehlin producing area of stomach is also removed, with the result that patient has satiety even after eating little bit of food and the person does not crave for food in between meals.
A procedure in which a stapling device is used to create a thin vertical sleeve of stomach about the size of a banana and the rest of the stomach is removed, thereby limiting the amount of food that can be eaten. It basically leaves a small stomach tube instead of a big stomach sack. The residual stomach capacity is about 150mls so a generous entry should be possible. Grehlin, which is an enzyme produced in the fundus of stomach, is responsible for hunger and craving for food. In this operation, Grehlin producing area of stomach is also removed, with the result that patient has satiety even after eating little bit of food and the person does not crave for food in between meals.
How Does the Sleeve Gastrectomy Cause Weight-Loss?
Sleeve gastrectomy is a restrictive procedure. It greatly reduces the size of the stomach and limits the amount of food that can be eaten at one time. It does not cause decreased absorption of nutrients or bypass the intestines. After this surgery, patients feel full after eating very small amounts of food. Sleeve gastrectomy may also cause a decrease in appetite. In addition to reducing the size of the stomach, the procedure reduces the amount of the “hunger hormone,” ghrelin, produced by the stomach. The duration of this effect is not clear yet, but most patients have significantly decreased hunger after the operation.
How Much Weight Loss Occurs After Sleeve Gastrectomy?
Several studies have documented excellent weight loss up to three years after Sleeve Gastrectomy. 3-6 In higher BMI patients who undergo Sleeve Gastrectomy as a first stage procedure, the average patient will lose 40–50 percent of their excess weight in the first two years after the procedure. This typically equates to about 125 pounds of weight-loss for patients with a BMI greater than 60. Patients with lower BMI’s who undergo Sleeve Gastrectomy will lose a larger proportion of their excess weight (60–80 percent) within three years of the surgery. Weight loss after Sleeve Gastrectomy has been directly compared to Laparoscopic Gastric Banding. In a randomized trial comparing Sleeve Gastrectomy to Gastric Banding, Sleeve Gastrectomy resulted in better weight-loss at three years (66 percent versus 48 percent excess weight-loss). Additionally, more than 75 percent of patients will have significant improvement or resolution of major obesity-related co-morbidities such as diabetes, hypertension, sleep apnea and hyperlipidemia following sleeve gastrectomy.
What are the Risks of Sleeve Gastrectomy?
The risk of major post-operative complications after Sleeve Gastrectomy is 5-10 percent, which is less than the risk associated with gastric bypass or malabsorptive procedures such as duodenal switch. This is primarily because the small intestine is not divided and reconnected during Sleeve Gastrectomy as it is during the bypass procedures. This lower risk and shorter operative time is the main reason we use it as a staging procedure for high-risk patients. Complications that can occur after Sleeve Gastrectomy include a leak from the sleeve resulting in an infection or abscess, deep venous thrombosis or pulmonary embolism, narrowing of the sleeve (stricture) requiring endoscopic dilation and bleeding. Major complications requiring re-operation are uncommon after sleeve gastrectomy and occur in less than 5 percent of patients
After the Procedure
You can probably go home 2 days after your surgery. You should be able to drink clear liquids on the day after surgery, and then a puréed diet by the time you go home. When you go home, you will probably be given pain pills or liquids and a medication called proton pump inhibitors. Your doctor, nurse, or dietitian will recommend a diet for you. Meals should be small to avoid stretching the remaining stomach.
